Introduction
Chronic musculoskeletal (MSK) pain is a common reason for referrals to pediatric rheumatology and can significantly impact a child’s physical, social, and academic life. One important cause of chronic, diffuse pain in children is pain amplification syndrome, often referred to as Amplified Musculoskeletal Pain Syndrome (AMPS). This condition functions as a pain phenomenon where the nervous system amplifies pain signals without any observable tissue damage. In pain amplification syndromes, mild stimuli (or even normal bodily sensations) are experienced as very painful, resulting in disproportionate pain complaints and functional disability. This guide offers outpatient pediatricians a broad overview of pediatric pain amplification syndrome: how to recognize it, differentiate it from other causes of MSK pain, initial evaluation steps, and management principles, all based on recent guidelines and literature from the past decade.
Understanding Pain Amplification in Children
Pain amplification syndrome is not a specific disease but a descriptive term that encompasses various chronic pain disorders in children, including juvenile fibromyalgia, complex regional pain syndrome (CRPS), and idiopathic (non-inflammatory) musculoskeletal pain. All these conditions share a common mechanism: abnormal processing of pain signals (often referred to as central sensitization), leading to heightened pain perception. In AMPS, normal pain pathways develop a “short circuit”—where pain signals trigger the autonomic nervous system, resulting in blood vessel constriction, reduced blood flow, and the buildup of metabolic waste in tissues, which in turn exacerbates pain in a vicious cycle. Importantly, the child’s pain is very real, even though it is “amplified” beyond what would be expected from any underlying injury or condition.
Typical profile: Pain amplification can affect children of all ages but is most commonly observed in pre-adolescents and adolescents, particularly among teenage girls. Children may report pain in either one area or multiple regions; it can be intermittent or constant. Often, these children appear otherwise healthy, although the pain may begin after a trigger such as an injury, illness, or significant stress. Commonly identified triggers include a prior injury or surgery, a viral illness (e.g., mononucleosis or the flu), or psychological stressors in the child’s life. A tendency toward joint hypermobility (very flexible joints) is also frequently observed and may predispose individuals to pain amplification. Many patients have a history of orthopedic injuries or “growing pains,” and some have family members with chronic pain issues, suggesting a potential genetic or learned predisposition component.
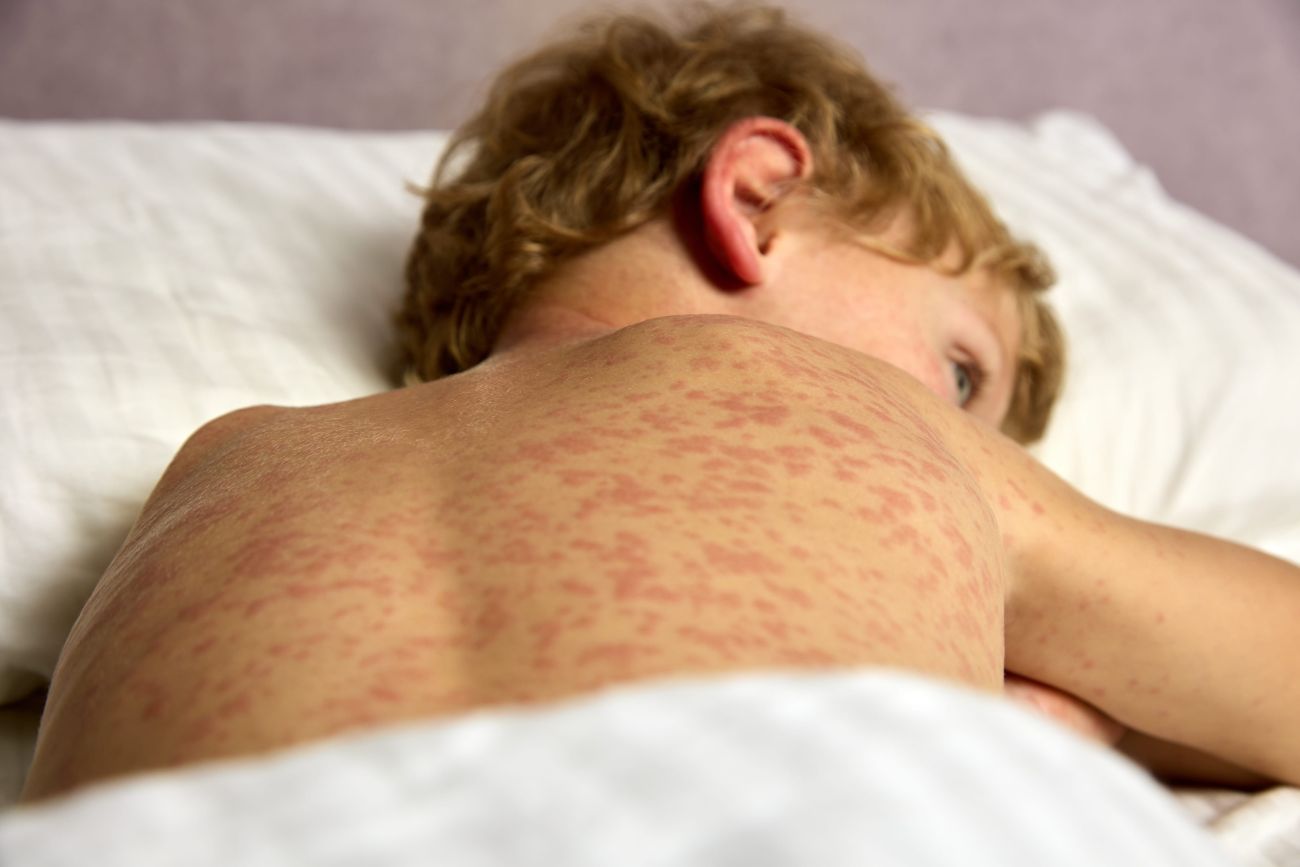
Clinical presentation: The hallmark of pain amplification syndrome is chronic pain that is often diffuse and disproportionate to any observable medical cause. Pain can occur anywhere—it may be localized (e.g., one limb) or widespread across multiple body regions. Affected children commonly describe a deep aching pain in their muscles or joints, sometimes accompanied by abnormal sensations like burning, tingling, or numbness. Pain amplification is also characterized by allodynia (pain from light touch) or hyperalgesia (an increased pain response to normally mild stimuli). On examination, there are typically no signs of inflammation (no joint swelling, redness, or warmth), and the musculoskeletal exam is generally normal aside from the pain response. Some children exhibit autonomic changes in the painful area, such as alterations in skin color or temperature, sweating, or cool extremities, particularly in CRPS (e.g., a limb might appear cold or mottled).
In addition to pain, children with amplified pain often experience a constellation of other symptoms:
Fatigue and poor sleep: Non-restorative sleep and chronic fatigue are quite common, often leaving children waking up feeling unrefreshed. Many struggle to maintain regular school attendance due to morning pain and fatigue.
Headache or abdominal pain: There may be concurrent headaches or chronic abdominal pain (functional abdominal pain), indicating a generalized pain sensitization.
Dysautonomia symptoms: Some patients experience symptoms such as dizziness (especially upon standing) or cold, discolored hands and feet similar to Raynaud’s phenomenon. These symptoms arise from autonomic nervous system involvement but are not dangerous.
Mood or psychosocial issues: Anxiety and depression can be present, either as contributing factors or as consequences of chronic pain. The stress of chronic pain and being misunderstood can intensify the pain experience. It’s important to note that psychological factors do not imply the pain is “fake’—rather, stress can trigger or worsen the pain through mind-body interaction pathways.
Children experiencing pain amplification often seem tired or weak, may hesitate to put weight on an affected limb despite normal imaging results, and can suffer significant functional impairment—such as missing school, avoiding sports or social activities, and becoming socially isolated. This loss of function is a defining characteristic; in contrast, children with purely mechanical pain (e.g., a specific sports injury) typically maintain normal function except for the particular activity that causes discomfort pain.
Initial Evaluation and Workup
When a child presents with chronic musculoskeletal pain, the first step is to perform a thorough history and physical examination to look for clues to other diagnoses. Pain amplification syndrome is primarily a diagnosis of exclusion—there is no specific test for it—and initial evaluation is aimed at ruling out inflammatory, infectious, malignant, or structural causes of pain.
History: Clarify the onset, duration, and pattern of the pain. Amplified pain typically has a subacute to gradual onset and has often been present for at least three months by the time of evaluation, as defined by juvenile fibromyalgia criteria. It may begin in one location and then spread, or its intensity may fluctuate over time. Inquire about triggers such as recent injuries, illnesses, or stressful events. Key historical “red flags” that suggest a move away from benign pain amplification and towards other pathology include: fever, weight loss, night sweats, pain that consistently disrupts the child’s sleep at night, focal bone pain in one area (especially without trauma), or morning stiffness lasting longer than 30 minutes (which could indicate inflammatory arthritis). Additionally, review any functional impact—such as an inability to attend school, ceasing sports activities, or needing assistance with daily tasks—since this helps assess severity. Children with amplified pain often have visited multiple providers and undergone various tests already; pay attention to prior normal investigations, as a trend of extensive normal workups is common before the diagnosis is made recognized.
Physical exam: Conduct a head-to-toe examination. In cases of pain amplification, objective findings are minimal. Joints have a normal range of motion (though the child may hesitate due to pain), and there is no swelling or warmth. The neurologic exam is typically normal, except for possible oversensitivity to light touch. Examine closely for signs of inflammation (such as swollen joints or rash), indicators of systemic disease (like lymphadenopathy or organomegaly), or focal tenderness over bones. Pay attention to the tender point exam: historically, fibromyalgia was linked with multiple predictable tender points on palpation. While tender points are no longer necessary for diagnosis, diffuse tenderness in various areas (without swelling) can support a pain amplification diagnosis. If pain is localized to one limb, assess for autonomic changes (such as color or temperature differences) that might indicate CRPS. Additionally, evaluate gait—children with amplified pain may limp or refuse to bear weight, although the limb appears anatomically normal (in CRPS, they might hold a limb protectively despite normal strength and reflexes). Growth and vital signs are typically normal; the presence of fever or growth failure suggests investigation into other causes causes.
Laboratory tests: In cases of pure pain amplification syndrome, routine laboratory tests typically show no significant findings. However, initial lab work remains essential to rule out inflammatory or malignant conditions. Reasonable first-line laboratory tests include:
Complete blood count (CBC) – checks for cytopenias or abnormal cells that might suggest leukemia, as well as for an elevated platelet count that may accompany inflammation or chronic stress.
Inflammatory markers (erythrocyte sedimentation rate (ESR) and C-reactive protein (CRP)) – these are usually normal or only mildly elevated in cases of amplified pain. A significantly elevated ESR/CRP indicates an inflammatory or infectious condition rather than simply pain amplification.
Muscle enzymes (CPK, aldolase) – if muscle weakness is observed during examination, they are tested to rule out myositis. In instances of pain amplification, weakness typically isn’t true muscle weakness but rather “give-way” pain-limited effort, and muscle enzyme levels will remain normal.
Autoimmune labs (e.g., ANA, rheumatoid factor) – not routinely necessary unless there is clinical suspicion of lupus or arthritis. An ANA test may often yield a positive result incidentally in children; routine screening for ANA is not advised without indications of rheumatologic disease. However, if joint swelling or other signs of autoimmune issues are present, relevant autoimmune tests should be performed.
Infection workup – If subacute bone pain is accompanied by low-grade fevers, testing for infections such as Lyme disease (in endemic areas) or others may be appropriate. Infection is less likely in typical cases of amplified pain without fever.
Imaging is guided by the clinical picture. X-rays of painful areas are often performed to exclude fractures or bone lesions. In cases of pain amplification syndrome, they are usually normal. If a child has persistent focal bone pain—particularly night pain or pain at rest in one location—advanced imaging may be needed; MRI can rule out bone tumors or osteomyelitis. An MRI for amplified pain is typically normal, although in some instances, specialists have observed changes such as bone marrow edema or vascular alterations on bone scans that suggest AMPS (e.g., in CRPS). However, these findings are not consistent or necessary for diagnosis. Essentially, imaging and lab tests for these patients often return normal results, which in itself can be a clue. It’s essential for the pediatrician to ensure that urgent and serious conditions are ruled out (for instance, if acute infection or malignancy is part of the differential diagnosis, the appropriate urgent evaluation should be pursued) before attributing symptoms to pain amplification. In practice, this means that if a child is acutely ill (high fever, severe focal pain, etc.), that condition should be managed first; pain amplification is considered only when symptoms are chronic and no other cause is identified evident.
Diagnostic challenges: Early in the course, not all features of amplified pain may be apparent. The syndrome can develop over time. It is not uncommon for these patients to undergo extensive evaluations by multiple specialists (orthopedics, neurology, etc.) before a unifying diagnosis is made. If you strongly suspect a pain amplification syndrome but are uncertain, it is reasonable to consult or refer to a pediatric rheumatologist early—rheumatologists are acquainted with the spectrum of these pain syndromes and can assist in confirming the diagnosis or guiding further testing. Remember that pain amplification is a diagnosis of exclusion: only after reasonable evaluation has not identified another cause, and the pattern aligns, should it be diagnosed.
Differential Diagnosis of Pediatric Musculoskeletal Pain
When a child presents with chronic musculoskeletal pain, consider a wide differential diagnosis. Pain amplification syndrome (functional pain) is located on the non-inflammatory end of the spectrum, and distinguishing it from other causes is essential to avoid overlooking serious conditions. Key differential diagnoses include:
Juvenile Idiopathic Arthritis (JIA): Chronic arthritis can lead to joint pain and morning stiffness, which may sometimes be mistaken for mere “aches.” However, JIA typically presents with clear signs of joint inflammation – such as swelling, warmth, and a limited range of motion in the affected joints – which are not present in cases of pure amplified pain. Children with JIA often experience worse pain in the morning that improves with activity, whereas amplified pain can be constant or may even intensify with physical activity. Inflammatory markers (ESR, CRP) may be elevated in JIA and other rheumatologic disorders. Furthermore, pain from JIA generally responds at least partially to NSAIDs or anti-inflammatory medications, whereas amplified pain shows little response to NSAIDs. If joint swelling, prolonged morning stiffness, or systemic symptoms (such as fever or rash) are present, inflammatory arthritis needs to be ruled out. Consult a pediatric rheumatologist if there is any suspicion of JIA, as early treatment is essential crucial.
Mechanical or Overuse Syndromes: Localized pain from orthopedic causes—such as Osgood-Schlatter disease (tibial tubercle pain in adolescents), patellofemoral pain syndrome, or muscle strains—can be common in active children. These pains are typically related to activity and localized (e.g., knee pain with running, heel pain with sports in Sever disease), improving with rest. This contrasts with amplified pain, which may persist at rest and be more widespread. The examination of mechanical pain often reveals focal tenderness (such as over the tibial tubercle) but no generalized allodynia. There are no systemic symptoms associated with simple mechanical pain. These conditions are generally managed with rest, ice, NSAIDs, and physical therapy, and they tend to improve over weeks to months. If a presumed “sports injury” pain is not improving as expected or becomes more diffuse, reconsider pain amplification or another issue cause.
Benign Hypermobility and “Growing Pains”: Benign joint hypermobility, common in some children and those with Ehlers-Danlos syndrome, can lead to musculoskeletal pain, particularly after exercise or at the end of the day. Hypermobile children may often experience musculoskeletal aches, yet typically have normal lab results and imaging. Their pain may overlap with pain amplification – indeed, hypermobility is frequently noted in patients with amplified pain – but hypermobility-related pain usually improves with targeted strengthening and does not cause the profound allodynia or functional impairment associated with AMPS. Growing pains (benign idiopathic nocturnal limb pains) are another consideration for younger children, typically aged 3 to 12. Growing pains result in deep leg pain, often located in the calves or thighs, occurring at night and resolving by morning, with no daytime complaints and a normal examination. They are self-limiting and not linked to the persistent, activity-limiting pain seen in amplification. Approximately 49% of children may experience benign growing pains, which only require reassurance and simple measures, such as heat or massage – they should not be confused with the chronic, daily pain of amplification syndromes.
Infection (Septic Arthritis or Osteomyelitis): These are acute conditions that can present with musculoskeletal pain, but the clinical picture is usually quite distinct from pain amplification. Septic arthritis or acute osteomyelitis typically shows severe localized pain, high fever, evident illness, and often an inability to use the affected limb. The joint involved is usually red, warm, very tender, and has limited range of motion due to pain. Lab tests reveal elevated inflammatory markers and often a high white blood cell count. These infections are emergencies that require prompt hospitalization, imaging, and intravenous antibiotics – they do not manifest as a long-standing diffuse pain syndrome. One caveat is indolent infections (such as subacute osteomyelitis or Kingella kingae arthritis in toddlers) can present with more subtle signs (mild fever, only slight lab elevations). Therefore, any acute-onset or localized bone/joint pain accompanied by fever should prompt an urgent evaluation to exclude infection before considering functional pain diagnosis.
Malignancy: Serious conditions such as leukemia or bone tumors (like osteosarcoma and Ewing sarcoma) can lead to bone and joint pain in children. Initially, pain from malignancy may be intermittent, but it often worsens over time and can occur at night, sometimes waking the child from sleep (night pain is a red flag). There may be additional signs: unexplained fevers, weight loss, fatigue, or pallor (in leukemia). On examination, there may be point tenderness in a bone. Laboratory findings may include cytopenias or extremely high inflammatory markers, but in the early stages of malignancy, these may still be normal, so a high index of suspicion is essential. A distinguishing feature is that patients with pain amplification often appear well otherwise, while a child with cancer may exhibit subtle signs of illness upon examination (such as pallor, lymphadenopathy, hepatosplenomegaly, etc.). If malignancy is a consideration, appropriate imaging (X-ray, MRI) and laboratory tests (including possibly LDH and uric acid for leukemia/lymphoma) should be performed promptly. Do not attribute unexplained persistent bone pain to “amplification” without ruling out malignancy, especially if any atypical features are present present.
Juvenile Fibromyalgia Syndrome (JFMS): Juvenile fibromyalgia essentially represents a form of widespread amplified pain. In practice, these terms overlap; diffuse amplified pain is frequently referred to as juvenile fibromyalgia. Classic fibromyalgia in children is characterized by chronic (greater than 3 months) widespread musculoskeletal pain, often accompanied by multiple tender points, fatigue, poor sleep, and frequently headaches or irritable bowel symptoms. Adapted diagnostic criteria for juvenile fibromyalgia, based on the 2010 American College of Rheumatology criteria for adults, include a Widespread Pain Index and Symptom Severity score. For general pediatricians, it is crucial to acknowledge that fibromyalgia is a legitimate diagnosis in adolescents and falls within the category of pain amplification syndromes, requiring similar management. Unlike inflammatory conditions, fibromyalgia and Amplified Musculoskeletal Pain Syndrome (AMPS) typically yield normal lab results and show no visible swelling. A tender point examination may still be beneficial; if a child experiences pain in at least 5 out of the 18 traditional tender point sites, fibromyalgia is likely. However, even if formal criteria are not completely satisfied, many children with chronic widespread pain will benefit from a similar approach as fibromyalgia.
Complex Regional Pain Syndrome (CRPS): CRPS (previously known as reflex neurovascular dystrophy or reflex sympathetic dystrophy in children) is a localized pain syndrome that typically affects one extremity following an injury. It is marked by severe limb pain accompanied by autonomic changes—the affected limb may appear swollen, sweaty, cold, or warm, with noticeable color changes. The pain often exceeds what would be expected from the initial injury, potentially resulting in the child not using the limb. CRPS has specific diagnostic criteria (the Budapest criteria) and is usually identified by these autonomic symptoms and the affected area. While it continues to be treated as an amplified pain condition (with physical therapy and desensitization playing key roles), due to its unique characteristics, CRPS cases are frequently co-managed with pain specialists or specialized programs. If a pediatrician suspects CRPS (evidenced by a child who has sustained a recent injury and is now experiencing debilitating limb pain along with swelling or color changes), it’s important to make an early referral to a pediatric pain clinic or rheumatology indicated.
In summary, pain amplification syndrome is considered when inflammatory, malignant, mechanical, and infectious causes have been reasonably excluded, and the clinical presentation aligns with a functional pain disorder: chronic, diffuse pain, a normal examination aside from pain behaviors, normal investigations, and often accompanied by fatigue or other somatic symptoms. Always maintain an open mind, and if something doesn’t seem to fit (for example, objective arthritis or fevers), investigate it further rather than labeling it as something else amplification.
Management in the Outpatient Setting
Management of amplified musculoskeletal pain in children is best approached through a biopsychosocial, multidisciplinary strategy. The goal is not only to relieve pain but also, importantly, to restore function and quality of life. As the primary care provider, a pediatrician can initiate first-line management while coordinating referrals to appropriate specialists. Key principles of treatment include patient and family education, physical rehabilitation, psychological support, and symptom management management.
1. Reassurance and Education: Begin by validating the patient’s experience—acknowledge that the pain is genuine. Explain, using age-appropriate language, the concept of pain amplification: that their nerves are functioning “too well” and sending pain signals even when there is no damage occurring. It is vital to stress that this pain, while real, does not indicate severe tissue damage or disease. This understanding helps to alleviate fear. Families should recognize that there is no immediate cure, but this condition can be managed and will improve over time with the right approach. Setting expectations is key: improvement is typically gradual. Encourage a focus on the long-term goal of returning to normal activities instead of seeking moment-to-moment pain relief. Often, simply receiving a diagnosis and knowing it’s not life-threatening brings relief and optimism to families.
2. Exercise and Physical Therapy: Exercise serves as the cornerstone of therapy for pain amplification syndromes. Numerous studies and guidelines (including those from the American Pain Society and EULAR) advocate for aerobic exercise as a first-line treatment for juvenile fibromyalgia and related conditions. The objective is to gradually recondition the body and desensitize the pain response. A pediatric physical therapist can develop a program of low-impact, moderate aerobic activities (such as swimming, cycling, or brisk walking) for at least 30 minutes, 2–3 times a week, increasing intensity as tolerated. Strength training or stretching exercises (like yoga, Pilates, or tai chi) can also be included for overall conditioning and flexibility. Early in treatment, exercise may cause increased discomfort – families should be prepared for this and encouraged to persist despite pain, as stopping due to discomfort reinforces the pain cycle. It’s important to emphasize that using the body normally will not result in damage, even if it causes pain. Over time, regular exercise enhances blood flow, diminishes the stress response, and elevates the pain threshold, leading to reduced pain intensity. Physical therapy sessions can also involve desensitization techniques for allodynia (for instance, gently rubbing the painful area with various textures to retrain the nerves). In addition, therapists will focus on posture, core strength, and addressing specific weaknesses, as deconditioning often accompanies chronic pain. A gradual return to sports or normal play as pain improves should be encouraged.
3. Cognitive-Behavioral Therapy (CBT) and Psychological Support: Considering the significant mind-body connection in amplified pain, psychological interventions are equally important as physical ones. CBT assists patients in developing coping strategies for pain, challenging negative thoughts (such as “my pain will never get better”), and managing stress or anxiety that can worsen pain. Other therapeutic methods, including acceptance and commitment therapy (ACT) or mindfulness-based stress reduction, can also be advantageous. Therapy can help address underlying issues (such as school stress, family dynamics, and mood disorders) and teach relaxation techniques (like deep breathing, guided imagery, and progressive muscle relaxation) to soothe the nervous system. It is advisable to involve a pediatric psychologist or pain therapist early on; these professionals can collaborate with the child and family on pacing activities, setting achievable goals, and overcoming the fear of pain. Family education is vital: at times, parents of children with chronic pain may understandably become overprotective; therapy can assist parents in supporting their child’s independence and activity despite pain, rather than inadvertently reinforcing disability. If anxiety or depression is substantial, therapy and, if necessary, a psychiatric evaluation for medications (such as SSRIs) should be included in the plan.
4. Sleep and Lifestyle: Focus on sleep hygiene and other lifestyle factors. Poor sleep increases pain sensitivity. Recommend consistent bedtimes, a calming pre-sleep routine, and avoiding electronics before bedtime. Treat conditions such as insomnia or restless legs if necessary. Good nutrition and maintaining a regular routine (attending at least part of the school day, if possible) are also beneficial—they provide structure and a sense of normalcy. Collaborate with the school if needed to develop a plan for the child to return to classes, perhaps starting with half-days or accommodations, with the goal of resuming full participation as their functional ability improves improves.
5. Medications: Medications play an adjunctive role in pediatric pain amplification and are often less effective in children compared to adults. There is no medication that “cures” amplified pain. However, specific medications can help alleviate symptoms and support other therapies:
- Analgesics: Simple analgesics, such as acetaminophen or NSAIDs, can be tried for pain flare-ups; however, as previously noted, heightened pain often does not respond significantly to NSAIDs. Avoid frequent or long-term use of NSAIDs unless they are clearly beneficial. Opioids should not be used, as evidence indicates they are ineffective for chronic functional pain and carry substantial risk.
- Neuropathic pain modulators: Low-dose tricyclic antidepressants (e.g., amitriptyline) or SNRIs (like duloxetine) and anticonvulsants (e.g., gabapentin, pregabalin) are commonly used in adults with fibromyalgia to assist with pain modulation and sleep. In children, the evidence is limited, but specialists might consider a trial of amitriptyline at bedtime (to aid sleep and pain) or gabapentin for those exhibiting significant neuropathic pain characteristics. Typically, these should be managed by or in consultation with a pediatric rheumatologist or pain specialist. If administered, initiate with a low dose and monitor for side effects (for instance, amitriptyline can cause drowsiness, which may actually be beneficial at night, but be cautious of potential cardiac side effects at higher doses) doses).
- Other medications: In certain situations, specialists may try a brief course of corticosteroids when there is uncertainty in the diagnosis (e.g., to determine if an inflammatory component is present – a lack of response might indicate a functional diagnosis). However, steroids are not a treatment for AMPS and are not indicated once the diagnosis is confirmed. Some teenagers with fibromyalgia and mood issues might benefit from SSRIs or anti-anxiety medications, but these also primarily address comorbid depression and anxiety rather than the pain directly.
It bears repeating that non-pharmacologic therapies are essential; medications, if utilized, only “support the other therapies and are generally not effective in children when used alone.” Many pediatric pain programs actually aim to reduce children’s reliance on any analgesics as they improve.
6. Multidisciplinary Pain Programs: If the child’s pain and disability are severe (for instance, if they are wheelchair-bound due to pain or have been absent from school for an extended period), consider referring them to a specialized interdisciplinary pain rehabilitation program. Pediatric amplified pain programs—often managed by departments of rheumatology or pain medicine—offer intensive physical therapy, occupational therapy, psychotherapy, and occasionally group therapy or educational tutoring in either an outpatient day program or an inpatient setting. Studies indicate that intensive interdisciplinary programs can significantly enhance function and reduce pain-related fear in children with amplified pain. However, most children can be effectively managed as outpatients with proper coordination among healthcare providers. The pediatrician’s role is to lead care coordination, ensure follow-up, and keep the child and family engaged and motivated therapies.
Prognosis: With appropriate treatment, the outlook for amplified pain syndromes in children is generally positive. Many patients regain normal function and experience significantly reduced pain over time. For instance, long-term follow-ups of children with CRPS who underwent intensive management reveal that the majority become fully functional and pain-free, with relatively low relapse rates. Children tend to respond and adapt better than adults with similar pain syndromes, likely due to shorter pain duration and greater plasticity in their coping mechanisms. However, some children may experience recurring episodes of pain amplification during periods of stress or as they transition into adulthood. Emphasize to families that developing resilience and self-management skills now will assist the child in overcoming future challenges. Regular exercise and stress management should become lifelong habits to sustain these improvements. Additionally, families should recognize that setbacks can occur – if pain increases again in the future, they should revert to the foundational strategies (and seek booster sessions in therapy or PT as needed) instead of feeling discouraged discouraged.
When to Refer and Specialist Consultation
Pediatricians handle numerous cases of musculoskeletal pain, but some circumstances require a referral to a specialist:
Diagnostic uncertainty or red flags: If you are uncertain whether the pain is amplified/functional or results from another disease, refer to a pediatric rheumatologist for evaluation. Any “red flag” findings (such as joint swelling, persistent fevers, abnormal lab results, or focal bone findings) should prompt a specialty referral. Rheumatologists are trained to distinguish amplified pain from inflammatory or autoimmune disorders and can expedite further workup if necessary.
Severe functional impairment: If pain leads to significant disability (such as frequent school absences or an inability to perform daily activities), a referral is indicated. Early involvement from a rheumatologist or pain clinic can aid in implementing a comprehensive program before the child falls too far behind in development or education.
Suspected CRPS: As noted, CRPS is most effectively co-managed with a pediatric pain specialist. If CRPS is suspected, particularly with significant autonomic changes, an urgent referral to a pain clinic or to a rheumatologist experienced in CRPS is essential recommended.
Lack of Improvement: If you have begun first-line interventions (education, basic PT, etc.) and after a few months there is no progress or the family is having difficulty with the plan, refer them to a specialist or multidisciplinary clinic. Sometimes the credibility of a specialist’s opinion or the resources of a specialty clinic (like dedicated physical therapists or psychologists) can jump-start progress.
Parental or patient anxiety: When a family is experiencing significant anxiety about the diagnosis or is not convinced that nothing serious is occurring, a rheumatology consultation can offer reassurance. Rheumatologists are able to conduct a thorough evaluation to confirm the diagnosis of pain amplification and reassure the family that conditions such as JIA or lupus are not present, which can encourage their commitment to the functional rehabilitation plan.
Whenever you are in doubt, it’s appropriate to involve a pediatric rheumatologist to discuss a case. Many institutions offer referral guidelines and even phone consultation lines. For instance, a pediatric rheumatology group suggests that patients should be evaluated when symptoms become a significant concern that affects school or activities. They encourage pediatricians to seek rheumatologists’ expertise for assistance in diagnosing or managing pain amplification syndrome. In summary, if the pain exceeds the ordinary and is confusing or debilitating, seek a support consult.
Conclusion
Musculoskeletal pain amplification syndrome in children is a diagnosis every general pediatrician should know, as it is a common cause of chronic pain referrals and can profoundly impact a child’s life. While it is a diagnosis of exclusion, recognizing the pattern of diffuse pain with normal objective findings can prevent unnecessary tests and interventions. Early identification and management of amplified pain by the primary care provider—through reassurance, appropriate workup, and the initiation of exercise and coping strategies—can shorten the course of disability and set the child on the path to recovery. Always maintain a broad differential to rule out other causes of MSK pain (such as JIA, infection, malignancy, and mechanical injuries), but once these are excluded, confidently explain pain amplification to families and begin the multidisciplinary treatment approach. By collaborating with pediatric rheumatologists, pain specialists, physical therapists, and psychologists, outpatient pediatricians can help children with pain amplification syndrome retrain their bodies and minds to move away from pain. The focus is on restoring function—getting the child back to school, play, and normal life—even before the pain fully resolves. With patience, support, and evidence-based strategies like exercise and CBT, most children will improve and can break the pain amplification cycle. Early referral in refractory or uncertain cases ensures that no serious condition is overlooked and that the child receives comprehensive care. Ultimately, recognizing that “pain amplification” is both a real and treatable condition will empower pediatricians to guide families through this challenging situation and help their patients reclaim a normal life childhood.
References and further reading
David D. Sherry: The Treatment of Juvenile Fibromyalgia with an Intensive Physical and Psychosocial Program. Journal of Pediatrics, 2015. https://doi.org/10.1016/j.jpeds.2015.06.036
Elizabeth L. Kaufman: Trends in Medicalization of Children with Amplified Musculoskeletal Pain Syndrome. Pain Medicine, 2017. https://doi.org/10.1093/pm/pnw188
Sabrina A. Gmuca: Fibromyalgia: Treating Pain in the Juvenile Patient. Paediatric Drugs, 2017. https://doi.org/10.1007/s40272-017-0233-5
Jessica W. Guite: Medication use among pediatric patients with chronic musculoskeletal pain syndromes at initial pain clinic evaluation. Pain Management, 2018. https://doi.org/10.2217/pmt-2017-0034
Susmita Kashikar-Zuck: Pilot Randomized Trial of Integrated Cognitive-Behavioral Therapy and Neuromuscular Training for Juvenile Fibromyalgia: The FIT Teens Program. The Journal of Pain, 2018. https://doi.org/10.1016/j.jpain.2018.04.003
Sabrina A. Gmuca: Opioid Prescribing and Polypharmacy in Children with Chronic Musculoskeletal Pain. Pain Medicine, 2019. https://doi.org/10.1093/pm/pny116
Sabrina A. Gmuca: The Role of Patient and Parental Resilience in Adolescents with Chronic Musculoskeletal Pain. Journal of Pediatrics, 2019. https://doi.org/10.1016/j.jpeds.2019.03.006
Sabrina A. Gmuca: Patient-proxy agreement on health-related quality of life in juvenile fibromyalgia syndrome. Pediatric Rheumatology, 2019. https://doi.org/10.1186/s12969-019-0320-y
David D. Sherry: The spectrum of pediatric amplified musculoskeletal pain syndrome. Pediatric Rheumatology, 2020. https://doi.org/10.1186/s12969-020-00473-2
Sabrina A. Gmuca: Suicidal risk and resilience in juvenile fibromyalgia syndrome: a cross-sectional cohort study. Pediatric Rheumatology, 2021. https://doi.org/10.1186/s12969-020-00487-w
L. Pianucci: Disordered eating among adolescents with chronic pain: the experience of a pediatric rheumatology subspecialty pain clinic. Pediatric Rheumatology, 2021. https://doi.org/10.1186/s12969-021-00506-4
Bernadette L. Dougherty: Longitudinal Impact of Parental Catastrophizing on Child Functional Disability in Pediatric Amplified Pain. Journal of Pediatric Psychology, 2021. https://doi.org/10.1093/jpepsy/jsaa127
Maitry Sonagra: Exploring the intersection of adverse childhood experiences, pediatric chronic pain, and rheumatic disease. Pediatric Rheumatology, 2022. https://doi.org/10.1186/s12969-022-00674-x
Sabrina A. Gmuca: Characterizing Neurocognitive Impairment in Juvenile Fibromyalgia Syndrome: Subjective and Objective Measures of Dyscognition. Frontiers in Pediatrics, 2022. https://doi.org/10.3389/fped.2022.848009
Anne M. Lynch-Jordan: Clinical Characterization of Juvenile Fibromyalgia in a Multicenter Cohort of Adolescents Enrolled in a Randomized Clinical Trial. Arthritis Care & Research, 2023. https://doi.org/10.1002/acr.25077