In pediatrics, weakness, fatigue, and malaise are frequently seen but they are nonspecific complaints. They can manifest as a general tiredness or as significant muscle weakness and exercise intolerance. A detailed evaluation is essential to differentiate between harmless causes and severe underlying conditions. This review provides a practical outpatient strategy aimed at general pediatric providers, focusing mainly on pediatric rheumatologic diseases and addressing other critical differential diagnoses. Essential steps include conducting a comprehensive history, performing a focused physical examination, ordering first-line labs or imaging, and identifying the appropriate circumstances for referral to pediatric specialists in rheumatology.
Common Rheumatologic Causes of Weakness, Fatigue, and Malaise
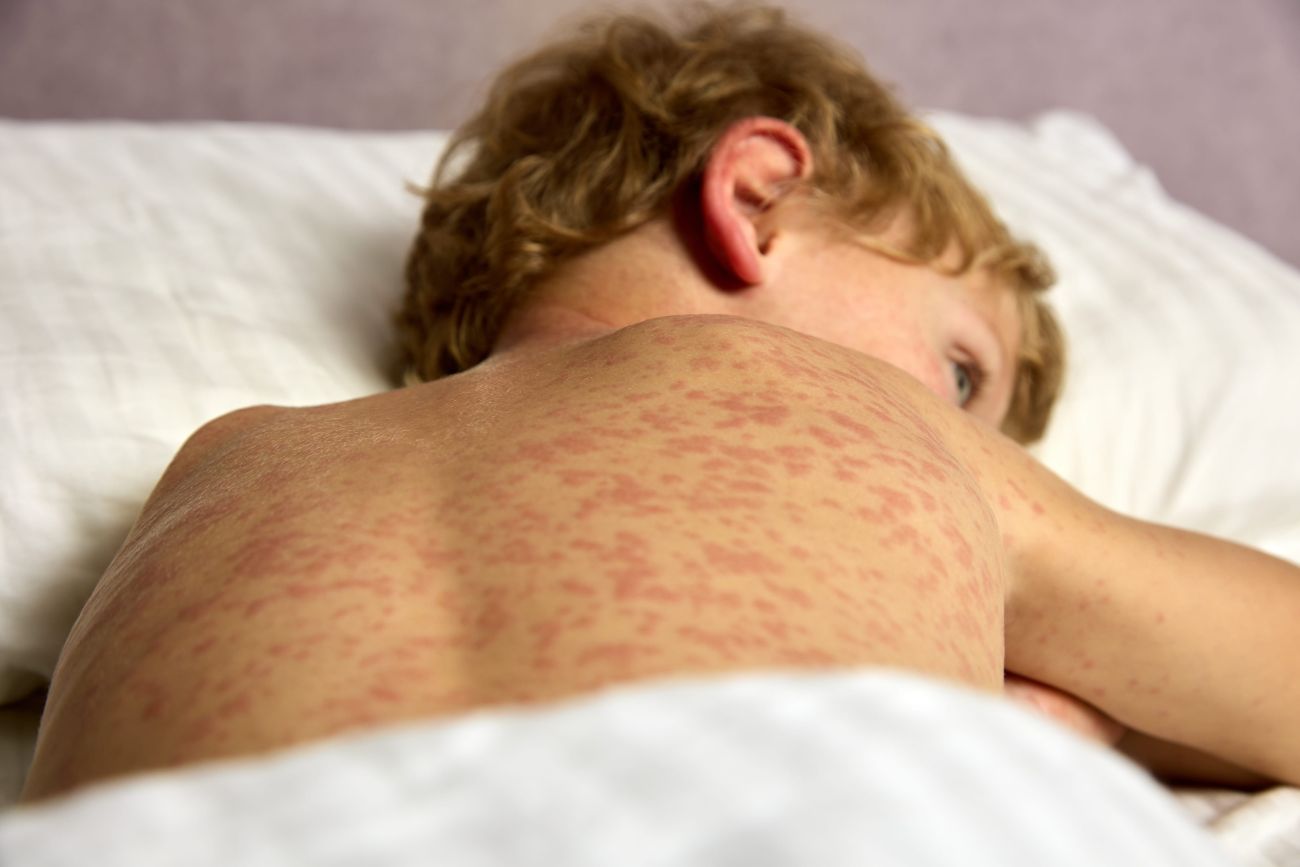
Systemic Lupus Erythematosus (SLE): SLE that begins in childhood often presents with vague constitutional symptoms. Among the earliest complaints in pediatric lupus are fatigue and malaise. Many patients may initially experience intermittent fever, weight loss, or a decreased appetite. Over weeks to months, more specific symptoms typically develop, such as a malar “butterfly” rash, oral ulcers, joint pain related to arthritis, kidney problems (like proteinuria), cytopenias, or serositis (pleuritis/pericarditis). As a multi-system autoimmune disease, SLE should be considered when a child exhibits any combination of unexplained fatigue with a rash, prolonged fever, or symptoms specific to organs (like the kidneys, blood, or CNS). Autoantibodies (like ANA, anti-dsDNA, etc.) are usually found to be positive, but their interpretation must be contextualized within the clinical scenario signs.
The butterfly rash (malar erythema) appears on the cheeks and nose in children with SLE. This acute and photosensitive rash notably spares the nasolabial folds, making it a classic indicator of lupus. Pediatric systemic lupus erythematosus (SLE) commonly presents with symptoms such as prolonged fever, malaise, fatigue, joint pain, and rash. Early indications may be subtle; therefore, it is crucial to remain vigilant if a child exhibits unexplained constitutional symptoms alongside any lupus-specific signs (including rash, oral ulcers, or proteinuria). Early identification is vital, as childhood SLE can be severe and may necessitate specialist intervention management.
Juvenile Idiopathic Arthritis (JIA): JIA is the most prevalent pediatric rheumatic disease, with chronic arthritis often leading to fatigue and an unwell appearance, even when joint symptoms are minimal. Most children with JIA report some level of fatigue, with approximately 15% experiencing moderate to severe fatigue. Contributing factors include chronic inflammation, poor sleep related to pain, and anemia associated with chronic disease. Fatigue is notably severe in systemic-onset JIA (Still’s disease), which typically presents with daily high fevers, a fleeting rash, lymphadenopathy, and significant malaise (the child looks unwell) before the emergence of arthritis. Polyarticular JIA (affecting multiple joints) may also result in considerable fatigue and weakness due to prolonged inflammation and muscle atrophy. Key historical and examination clues involve morning stiffness, joint swelling or stiffness lasting more than six weeks, limping, or refusal to bear weight. Even if the child appears generally healthy, ongoing joint pain (especially with swelling) during examination is concerning. JIA subtypes can usually be identified based on their patterns (e.g., oligoarticular versus polyarticular) and extra-articular symptoms (such as fever, rash, or uveitis). Laboratory tests for JIA often yield nonspecific results, including mild anemia and elevated inflammatory markers (ESR), with the potential presence of positive ANA or rheumatoid factor in specific subtypes, making the diagnosis primarily clinical. In summary, consider JIA in any child experiencing chronic fatigue accompanied by musculoskeletal complaints, particularly morning joint stiffness or swelling.
Juvenile Dermatomyositis (JDM): JDM is an inflammatory myopathy leading to proximal muscle weakness and systemic symptoms. Children with JDM typically experience gradually worsening weakness, including difficulty with activities such as climbing stairs, rising from the floor, or combing their hair, low energy (fatigue), and a general feeling of unwellness (malaise). Key characteristic skin findings help identify JDM: a heliotrope rash (a violaceous discoloration of the eyelids) and Gottron papules, which are scaly red-purple plaques found on the extensor surfaces of the finger joints, elbows, or knees. JDM usually manifests in children aged 5 to 14. During an examination, look for symmetric proximal muscle weakness affecting the neck, shoulder, or hip girdle and distinctive rash lesions. Laboratory indicators of the condition often include elevated levels of muscle enzymes (CK, AST/ALT, LDH, aldolase), which reflect muscle inflammation. Although a definitive diagnosis might require an MRI or muscle biopsy, in an outpatient context, recognizing the clinical triad of weakness, fatigue/malaise, and rash should lead to an urgent referral to rheumatology.
Gottron papules appear on the knuckles of a child diagnosed with juvenile dermatomyositis. These raised, scaly, red plaques found on the extensor MCP/IP joints are characteristic of dermatomyositis. JDM leads to progressive weakness in the proximal muscles and fatigue; hence, children may struggle to climb stairs or rise from a seated position. Any child exhibiting noticeable muscle weakness during an examination should be assessed for inflammatory myositis, primarily if accompanied by such rash symptoms. Timely treatment can avert severe complications such as muscle damage, calcinosis, and difficulty swallowing.
Other pediatric rheumatic disorders: Rarer connective tissue and autoinflammatory diseases may also manifest with fatigue/malaise:
Vasculitides: Systemic vasculitis is uncommon in children but crucial to identify. For instance, Takayasu’s arteritis, a type of large-vessel vasculitis, may lead to chronic fatigue, joint pain, and possibly limb claudication; a key examination finding is the absence of peripheral pulses in adolescents. ANCA-associated vasculitis, such as granulomatosis with polyangiitis in teenagers, can result in weight loss, fatigue, and specific organ-related symptoms (e.g., chronic sinusitis, pulmonary or renal issues). Henoch-Schönlein purpura (IgA vasculitis) and Kawasaki disease are more acute and typically evident by their distinctive rash, fever, and organ involvement, making chronic fatigue presentation less likely.
Mixed Connective Tissue Disease (MCTD) and Overlap Syndromes:** Children may occasionally exhibit overlapping lupus, dermatomyositis, and scleroderma characteristics. Such patients frequently experience fatigue and weakness alongside various signs (Raynaud phenomenon, arthritis, rash, etc.). High titers of U1-RNP antibody can indicate MCTD.
Juvenile Scleroderma: Systemic sclerosis in children is infrequent. Localized scleroderma (morphea) does not lead to widespread fatigue. However, systemic sclerosis may cause fatigue, skin tightening, Raynaud’s phenomenon, and organ complications (e.g., gastrointestinal, lung).
Periodic Fever Syndromes: Autoinflammatory syndromes (e.g., FMF, TRAPS, CAPS, PFAPA) can manifest as recurrent fever episodes, malaise, and fatigue. Between flare-ups, children generally feel well. If there is a history of recurrent unexplained fevers with systemic symptoms, consider these conditions and refer for further evaluation.
Juvenile Fibromyalgia / Chronic Pain Syndromes: Although it is not an autoimmune disease, pediatric rheumatologists often manage conditions such as juvenile fibromyalgia or amplified musculoskeletal pain. Fibromyalgia typically affects adolescents, being more common in girls and rarely occurring before puberty. It causes chronic, widespread musculoskeletal pain, poor sleep, and significant fatigue. There are no inflammatory signs; the exam may reveal tender points but shows normal strength and lab results otherwise. It’s a diagnosis of exclusion once other causes of fatigue and pain are ruled out. If suspected, a referral can assist with multidisciplinary management strategies, including exercise, sleep hygiene, and therapy.
Important Non-Rheumatologic Differential Diagnoses
Before attributing fatigue or weakness to a rheumatic condition, outpatient pediatricians should consider common non-rheumatologic causes. Infections are a frequent culprit—Epstein-Barr virus (mononucleosis), CMV, parvovirus B19, and post-COVID syndrome can all lead to prolonged fatigue. Chronic infections like tuberculosis, HIV, or hepatitis B/C are rare but essential, especially when risk factors or constitutional symptoms (weight loss, night sweats) are present. Testing should be guided by history and exam—routine broad viral panels or serologies (e.g., EBV, Lyme) are discouraged due to low yield and high false positives.
Endocrine and hematologic conditions also warrant early evaluation. Hypothyroidism, adrenal insufficiency, and diabetes mellitus can all cause fatigue with subtle early signs. The initial workup should include a basic lab panel including TSH, free T4, glucose, and electrolytes. Anemia—especially iron deficiency—is common and treatable. More serious causes like hemolytic anemia or malignancy (leukemia, lymphoma) should be considered in children with pallor, bruising, bone pain, or lymphadenopathy. True weakness (not just low energy) may suggest neuromuscular or neurologic disorders such as muscular dystrophies, myopathies, peripheral neuropathies, or central lesions and warrants referral.
Lastly, fatigue may stem from cardiovascular, pulmonary, or psychosocial causes. Undiagnosed heart disease, uncontrolled asthma, or obstructive sleep apnea can limit exercise and disrupt sleep. In adolescents, mood disorders like depression and anxiety are common contributors, often with somatic complaints. Sleep deprivation, deconditioning, and poor nutrition (e.g., vitamin D deficiency) can also play a role. A thorough psychosocial and lifestyle assessment is essential, and a mental health referral should be considered if functional or psychological fatigue is suspected.
Note: Laboratory testing for infections should be guided by history and exam. Broad viral panels are usually low-yield. In fact, guidelines advise against indiscriminate serologic testing for EBV, CMV, or Lyme in chronic fatigue workups, as positive titers are common and often do not change management. Instead, focus tests on those infections that clinical clues point toward.
Initial Outpatient Workup: Step-by-Step Approach
A systematic approach helps ensure no key detail is missed. Below is a step-by-step guide to evaluating a child with weakness, fatigue, or malaise in the outpatient setting:
History: Characterize the Fatigue/Weakness and Look for Clues
Take a detailed history to narrow the differential. Important elements include:
Onset and Duration: When did the symptoms begin, and were they triggered by anything? Acute onset (days to a week) suggests infection or acute illness, while chronic (>1–3 months) points to chronic disease or functional causes. In the absence of red flags, transient fatigue lasting less than 1 month often resolves on its own (e.g. post-viral).
Severity and Course: Is the fatigue constant or intermittent? Is it worsening, improving, or fluctuating? For example, daily cyclic fevers paired with evening fatigue suggest systemic JIA, whereas episodic fatigue with fevers may indicate a periodic fever syndrome.
Weakness vs. Fatigue: Clarify what the child or parent means by “weak” or “tired.” Inquire whether the child can physically keep up with their peers, climb stairs, or carry their backpack. True muscle weakness, characterized by difficulty lifting objects, frequent falls, trouble swallowing, or inability to hold up the head, should be distinguished from generalized low energy. Easy fatigability, such as muscles tiring after brief exercise, may indicate neuromuscular junction issues or myopathy.
Associated Symptoms:
- Fever or Weight Loss: Chronic low-grade fevers or unexplained weight loss are red flags for inflammation, infection, or malignancy.
- Pain: Any joint pain, swelling, or morning stiffness can suggest JIA or lupus arthritis. Muscle pain with weakness may suggest myositis or fibromyalgia. Bone pain, especially night pain or limping, raises concerns for leukemia, bone tumors, or chronic recurrent osteomyelitis.
- Rashes or Skin Changes: Ask about any rash (location, timing). Specifically, inquire about rashes on the cheeks (malar rash), eyelids, knuckles (dermatomyositis), photosensitivity rash, hives, livedo reticularis, bruising, etc. Note any hyperpigmentation (Addison’s), ecchymoses/petechiae (low platelets or leukemia).
- Lymph Node Swelling: Generalized lymphadenopathy could indicate infection or malignancy.
- Sore Throat or Recurrent Infections: Mono often begins with a severe sore throat. Frequent infections suggest immunodeficiency or could simply result from daycare exposure.
- Respiratory: Symptoms such as cough, wheezing, chest pain, or shortness of breath during exertion may indicate cardiopulmonary issues.
- GI: Chronic abdominal pain, diarrhea, or bloody stools (consider IBD), vomiting (may suggest Addison’s or increased intracranial pressure), and mucosal ulcers (could indicate Crohn’s or lupus).
- GU: Changes in urination (polyuria in diabetes, hematuria in lupus, dysuria in UTI).
- Neurologic: Headaches, vision changes (e.g., double vision in myasthenia or blurred vision in MS), muscle cramping, numbness/tingling, and back pain (may relate to spinal cord issues).
- Psychological: Changes in mood, sleep disturbances, stressors, or alterations in school performance.
- Recent Illnesses and Exposures: If weakness follows any recent viral illness, it might support the diagnosis of post-viral fatigue or GBS. Tick bites could imply Lyme disease, and travel may suggest exposure to endemic infections or TB. Consider any new medications that cause sedation or myopathy (like isotretinoin or high-dose steroids) and toxin exposures (lead poisoning can result in anemia and fatigue).
- Family History: A family history of autoimmune diseases (such as lupus, rheumatoid arthritis, or thyroid disease) raises suspicion in the patient. History of neuromuscular diseases (like Duchenne in maternal male relatives) or mental health issues should also be noted.
- Social History: Inquire about school attendance (have they been missing school?), academic or peer stress, sleep patterns (bedtime, wake time, use of electronics at night), diet, and exercise habits. Assess the potential for drug or alcohol use in teens, as substance use can lead to fatigue or signify depression.
- Impact on Life: Ask how fatigue or weakness affects daily activities—for example, “Can you play through a soccer game?” or “Does your child take naps, and did they before?” The need for naps or trouble keeping up with play can quantify the fatigue. Deteriorating school performance may be an early indicator of hypothyroidism or concentration issues stemming from fatigue.
❗❗❗❗
Red flags from history that suggest serious causes include unintentional weight loss, persistent or high fevers, night sweats, severe pain, limitation of activities, confusion or decline in school function, and any focal neurologic symptoms. If these are present, pursue an aggressive workup for organic disease.
Physical Examination: Look for Objective Findings
Perform a thorough head-to-toe exam, focusing on corroborating any historical clues and searching for “hidden” signs of systemic disease:
Vital Signs: Particularly note fever (even low-grade), tachycardia (which could indicate anemia or dehydration), bradycardia (which can be seen in hypothyroidism), and blood pressure (orthostatic hypotension in adrenal insufficiency or dysautonomia). Plot height and weight percentiles—crossing percentiles downward may indicate chronic illness or malnutrition.
General Appearance: Does the child look well or ill? A child with severe systemic disease often appears unwell or has low energy in the exam room. However, some children with mild JIA or isolated anemia may appear well. If the child looks acutely toxic or severely ill, that may warrant hospital evaluation rather than continued outpatient workup.
Skin: Inspect for rashes or lesions:
- Malar rash on cheeks/nose, photosensitive rash or discoid lesions (suggest SLE).
- Heliotrope purple rash on eyelids or Gottron papules on knuckles (dermatomyositis).
- Petechiae or purpura (if in distal extremities, it could be vasculitis like HSP; if it is widespread with bruises, think thrombocytopenia or leukemia).
- Erythema nodosum (tender red nodules on shins – can be TB, IBD, or infection-related).
- Eczema or atopic stigmata (Dennie-Morgan eye folds, xerosis) if the complaint might be related to poor sleep from itching.
- Vitiligo or mucocutaneous candidiasis (suggest autoimmune polyendocrine syndrome with Addison’s).
- Nasal or oral ulcers: Painless oral ulcers suggest SLE; painful canker sores could be IBD or PFAPA syndrome; nasal ulcers can occur in Wegener’s granulomatosis.
- Hair loss (alopecia): Patchy hair loss can be caused by lupus or dermatomyositis, while diffuse thinning might be caused by hypothyroidism or telogen effluvium from severe illness.
- Hyperpigmentation: Observe the gums, palms, and scars – diffuse bronzing suggests Addison’s disease.
- Scars or track marks: In teenagers, self-harm cuts or injection marks may indicate depression or drug use.
Lymph Nodes: Assess the cervical, axillary, and inguinal lymph nodes. Significant generalized lymphadenopathy, defined as more than two noncontiguous sites being enlarged, raises concern for potential infections, such as EBV, HIV, or malignancy. Tender nodes are more likely to be reactive or infectious, while hard or matted nodes may suggest further issues with lymphoma.
HEENT: Check the conjunctiva for pallor (anemia). Examine the sclera for icterus (hemolysis or liver disease). Perform a fundoscopic exam if there is concern about increased intracranial pressure (e.g., headaches). Assess the oropharynx for tonsillar hypertrophy (risk of OSA), thrush (possibly due to HIV or steroid use), and ulcers (as mentioned above). Palpate the thyroid gland for enlargement or nodules (hypo/hyperthyroid).
Chest: Auscultate the heart for murmurs, as anemia can cause flow murmurs, and congenital heart disease may have unrecognized murmurs. Check lung fields for crackles, which may indicate interstitial lung disease, heart failure, or wheezes (asthma).
Abdomen: Examine for hepatosplenomegaly – an enlarged spleen or liver in a fatigued child is a significant red flag (it could indicate leukemia or lymphoma, storage diseases, chronic active hepatitis, or systemic JIA). Also, observe for any masses. Mild liver enlargement might also be related to heart issues failure.
Musculoskeletal Exam: Use the pGALS screening exam (pediatric Gait, Arms, Legs, Spine) or a similar systematic approach:
- Joints: Inspect all major joints for swelling, warmth, or a limited range of motion. Even if no pain is reported, painless joint swelling, especially in the knees, can sometimes be present in chronic JIA. Look for effusions in the knees and ankles and swelling in the small joints of the hands. Any joint contracture or deformity indicates long-standing arthritis.
- Spine: Examine flexibility and tenderness in the SI joint (reduced flexion or pain may suggest) spondyloarthropathy).
- Gait: Observe the child walking or running if age allows. A limp or refusal to bear weight is significant. Gowers’ maneuver: if the child is young, ask them to get up off the floor and observe whether they push off their legs, which is a sign of proximal weakness.
- Muscle strength: Evaluate upper and lower extremity strength against resistance. Concentrate on proximal muscles (shoulder abduction, hip flexion) as these are frequently impacted in myositis or muscular dystrophy. In JDM, proximal weakness may be subtle without formal testing. Assess neck flexor strength (which is often diminished in myopathies). Distal strength (hand grip, foot dorsiflexion) helps confirm that peripheral nerves are intact (distal weakness with areflexia might suggest neuropathy).
- Muscle bulk: Check for muscle atrophy (for example, flattened thigh muscles may occur in JDM or if a limb is underused due to arthritis). Calf hypertrophy (pseudohypertrophy) in a young boy suggests Duchenne muscular dystrophy.
- Tenderness: Any focal bony tenderness, particularly over long bones, may indicate leukemia or chronic osteomyelitis. If there is widespread pain, generalized fibromyalgia tender points might also be noted but not diagnostic.
Neurologic Exam: Evaluate deep tendon reflexes in the arms and legs. Hyperreflexia accompanied by weakness indicates CNS lesions, while hyporeflexia or areflexia with weakness suggests peripheral nerve or muscle issues (e.g., GBS, CIDP, neuropathy). Test balance using the Romberg test and assess cerebellar function, mainly if there are complaints of dizziness or weakness that could be neurologic. Examine cranial nerves: ptosis or ophthalmoplegia may indicate neuromuscular junction disorders (such as myasthenia gravis or botulism in infants). Ensure that the sensation appears to be grossly intact. If the child reports dizziness or palpitations upon standing, measure orthostatic vitals (which could indicate POTS or dehydration).
Genital exam: In adolescent girls experiencing fatigue, consider heavy menstrual bleeding a potential cause of iron deficiency anemia; inquire about pallor or dizziness during menstruation. An exam is typically unnecessary unless abuse or other concerns are suspected, but the history is crucial.
Mental status: Observe the child’s affect and engagement. A child who appears apathetic or has a flat mood may be experiencing depression. An anxious, fidgety child might be struggling with anxiety or hyperthyroidism. Cognitive function is generally intact during fatigue, but any confusion or memory issues in a teenager could indicate potential lupus brain involvement or severe depression.
Document all findings. The physical exam will frequently yield crucial clues—such as discovering an enlarged spleen or a subtle rash, which can completely redirect the workup.
Initial Laboratory Investigations
After taking the history and exam, order a focused set of first-line laboratory tests to screen for common causes. A reasonable initial lab panel for a child with fatigue or malaise (without an obvious diagnosis) includes:
Complete Blood Count (CBC) with differential: Check for anemia (low hemoglobin) and its characteristics (microcytic vs. macrocytic), along with white blood cell count (infection or leukemia) and platelet count. For instance, anemia and thrombocytopenia may raise concerns for leukemia or lupus; leukocytosis and thrombocytosis are associated with inflammation (e.g., systemic JIA). A normal CBC is reassuring but doesn’t rule out all illnesses (as noted, leukemia can sometimes present with a near-normal CBC in the early stages).
Inflammatory markers: Erythrocyte Sedimentation Rate (ESR) and/or C-reactive protein (CRP). These are general indicators of inflammation. An elevated ESR/CRP indicates an underlying inflammatory or infectious process (e.g., rheumatic disease, chronic infection, IBD, malignancy) rather than simple psychosomatic fatigue. Significantly high ESR (along with elevated platelets) often suggests active inflammation (such as a JIA flare); extremely high ferritin alongside inflammation may indicate systemic JIA or macrophage activation syndrome. In contrast, a completely normal ESR/CRP is frequently observed in cases of functional fatigue or fibromyalgia, although mild lupus or mild JIA can also present with normal ESR.
Metabolic panel: A basic metabolic panel (BMP) or comprehensive metabolic panel will evaluate electrolytes, kidney function, and liver enzymes. This can identify dehydration, kidney issues, or liver inflammation. Liver enzymes (AST/ALT) can also be raised in muscle disease (as they are released from muscle). If AST/ALT levels are disproportionately elevated compared to other liver markers, consider muscle (and check CK). Elevated creatinine may indicate renal failure and fatigue; low bicarbonate could suggest acidosis in cases of adrenal insufficiency.
Muscle enzymes: CK (creatine kinase) and possibly aldolase should be considered, mainly if weakness is a symptom. A high CK level (often thousands) suggests muscle breakdown (myositis, dystrophy, rhabdomyolysis). JDM typically shows CK levels greater than 10–50 times the normal range. Muscular dystrophies in toddlers can present with significantly elevated CK levels even before noticeable weakness occurs. If CK is normal and true weakness is observed, muscle pathology is less likely, with neuropathy or a central cause being more probable.
Thyroid function: TSH and free T4 should be included to screen for hypothyroidism (elevated TSH, decreased T4) or, less commonly, hyperthyroidism (low TSH, elevated T4, which can also cause fatigue, weight loss, and anxiety). Thyroid disease is a crucial, treatable cause of fatigue in children.
Iron studies: At least check serum ferritin (an acute phase reactant, but also low in iron deficiency) or iron, TIBC, and transferrin saturation if anemia is present or if the patient is a menstruating teenage girl, even without anemia (iron deficiency can cause fatigue before anemia develops). If ferritin is low or iron saturation is low, it confirms iron deficiency.
Vitamin levels (selected): Not every child requires vitamin testing, but if there are concerns in the dietary history or if anemia is macrocytic, it’s important to check vitamin B12 and folate levels. If there is bone pain or risk factors for low vitamin D, it’s advisable to check 25-OH vitamin D, although empirical supplementation can be considered if suspicions are high. Vitamin D deficiency is common, and addressing it benefits bone health, even though its direct role in fatigue remains debated.
Urinalysis: A simple urine dipstick can detect blood or protein, which may be the first indication of lupus nephritis, kidney disease, or glucose, which relates to diabetes. In a fatigued adolescent, urine analysis is a quick screening tool for renal involvement or diabetes.
Autoimmune markers: These may be considered if there is clinical suspicion of rheumatologic disease based on history or examination:
Antinuclear antibody (ANA): A screening test for lupus and other connective tissue diseases. Use ANA judiciously – if the pre-test suspicion is low (no specific signs of autoimmunity), an ANA can often be false-positive and cause confusion. However, if there are features like rash, arthritis, or serositis suggestive of lupus or juvenile dermatomyositis, an ANA is reasonable. A strongly positive ANA (especially at high titer) in a child with fatigue and other symptoms warrants further lupus evaluation (dsDNA, Smith antibody, etc.). Reminder: A positive ANA alone (with no clinical signs) should not prompt rheumatology referral – many healthy children have low-titer ANA.
Lupus panel: If ANA is positive or clinical lupus features are present, order anti-dsDNA, anti-Smith, antiphospholipid antibodies, and C3/C4 complement levels. These can help confirm SLE. Low complements with positive dsDNA support lupus.
Rheumatoid factor (RF) and anti-CCP antibodies are positive in only a minority of JIA cases (RF is usually only positive in teenage-onset poly JIA, which resembles adult RA). They’re not routine screening tests for all fatigue, but checking them can be helpful if chronic polyarticular joint swelling is present.
HLA-B27: If suspecting a spondyloarthropathy (teen with chronic back pain, stiffness, or recurrent enthesitis), HLA-B27 testing might be done. It’s positive in >80% of ankylosing spondylitis and related disorders.
Creatine phosphokinase (CPK): Already mentioned – essential if muscle weakness is present. (Included under muscle enzymes above).
ESR/CRP: (already mentioned under inflammatory markers).
Infection-focused tests: Only if indicated by specific suspicions:
- Monospot test or EBV serology: If the history strongly suggests mononucleosis (acute onset, lymphadenopathy, sore throat, enlarged spleen) and it’s still early in the course, a Monospot (heterophile antibody test) can confirm EBV infection. Remember that Monospot results can be false-negative in young children or early in the illness, so an EBV-specific antibody panel (VCA IgM, etc.) might be sent if the initial Monospot is negative but suspicion remains high. Do not send EBV serologies for every fatigued child—only if the signs point to mono.
- A throat culture or rapid strep: If a sore throat is present—chronic fatigue could rarely be due to chronic Strep (the PANDAS theory is controversial), but it’s more likely that the child has had repeated strep infections and potentially post-strep glomerulonephritis (with fatigue arising from renal issues). This testing mainly aims to rule out a current infection.
- TB tests: As mentioned, if there is a TB risk (such as contact, travel, or immunocompromised status) or symptoms like a prolonged cough or weight loss, conduct a PPD or IGRA to rule out tuberculosis. Additionally, if starting immunosuppressive therapy is being considered (for example, if there’s a high suspicion of JDM requiring steroids), a baseline TB test is advisable.
- HIV test: If risk factors are present (mother HIV-positive, unknown status, or high-risk behaviors in a teen), include an HIV test.
- Lyme titer: Only request if there is a history of tick exposure, knee arthritis, etc. Routine Lyme testing for nonspecific fatigue is discouraged.
Additional tests based on the exam:
If renal or liver function is abnormal, further tests (renal ultrasound, hepatitis serologies, etc.) may be necessary. If inflammatory bowel disease (IBD) (GI symptoms, anemia, high platelets) is suspected, consider a stool occult blood test, calprotectin, or GI referral for endoscopy. If celiac disease is possible (chronic fatigue, iron deficiency, +/- GI symptoms), check tissue transglutaminase IgA and total IgA levels. If there are signs of hemolysis (jaundice, high LDH, low haptoglobin), perform a Coombs test. Ferritin can serve as both an iron marker and an inflammatory marker; very high ferritin levels, fatigue, and fevers may indicate systemic JIA or MAS.
Bone marrow biopsy/aspiration: Leukemia or bone marrow failure is strongly suspected (abnormal CBC or exam), so this diagnostic procedure would be necessary via a hematology referral.
In summary, the initial lab workup covers a broad range of common issues: anemia, inflammation, thyroid problems, etc. Many of these tests will return normal results in numerous children experiencing fatigue. Suppose all initial tests return normal and no concerns are noted during the examination. In that case, it is reasonable to provide supportive observation for a short time while promoting good nutrition, sleep, and exercise—especially if the fatigue has persisted for a brief period (less than 1 to 2 months). However, if lab results show any abnormalities, or if there is still a strong clinical suspicion for a condition despite normal test results, proceed with more focused second-tier tests or referrals as appropriate.
Imaging Studies: When and What to Order
Imaging is unnecessary in every case of pediatric fatigue, but it becomes important if specific findings warrant it. Use imaging to clarify suspicions from the history/exam:
X-rays: Obtain plain radiographs if localized bone or joint symptoms are present. For example:
- A joint X-ray can confirm an effusion or erosion in JIA and rule out orthopedic causes such as fractures, osteochondromas, or osteomyelitis. Long-standing arthritis may display joint space narrowing or growth disturbances.
- Chest X-ray: If respiratory symptoms are present or if TB is suspected this test can be used as a baseline to check for hilar lymphadenopathy. In cases of systemic JIA with prolonged fever, a CXR can assess for complications of macrophage activation syndrome, such as pericardial effusion.
- Bone pain: X-ray of the affected bone to investigate for tumors like osteosarcoma, which may exhibit a periosteal reaction, chronic osteomyelitis, or stress fractures.
- Sinus X-ray or preferably a sinus CT: If there is chronic sinus tenderness suggesting possible Wegener’s granulomatosis, although it is a rare concern).
Ultrasound: Useful for joint evaluation in kids (no radiation). If a joint exam is equivocal, an ultrasound can detect synovial effusions or synovitis in knees, ankles, or hips. For example, hip ultrasound if a toddler refuses to walk (to distinguish transient synovitis vs. septic arthritis vs. JIA).
Echocardiogram: If exam findings suggest possible cardiac cause (murmur, gallop, hepatomegaly) or if the fatigue is accompanied by syncope or chest pain on exertion, get an echo to evaluate cardiac function and rule out myocarditis or cardiomyopathy.
Electrocardiogram (ECG): If palpitations or syncope are present, check for arrhythmias or heart block (e.g., third-degree heart block can manifest neonatal lupus if congenital or Lyme carditis in teens with fatigue and AV block).
MRI: This is particularly helpful in suspected musculoskeletal or neurologic cases:
- MRI of affected muscles: In cases of suspected juvenile dermatomyositis or polymyositis, MRI (particularly MRI STIR sequences) of the thigh or pelvic girdle muscles can reveal muscle edema (inflammation) and guide biopsy decisions. Some centers perform an MRI to confirm myositis before beginning therapy, as it is non-invasive.
- MRI of joints (with contrast): If spondyloarthritis is suspected (evidenced by low back pain and stiffness in a teenager), an MRI of the sacroiliac joints can identify sacroiliitis earlier than X-rays. In juvenile idiopathic arthritis (JIA), an MRI of an affected joint may reveal synovitis or damage not visible on X-rays.
- MRI of the brain/spine: If neurologic red flags are present (such as focal deficits, severe headaches, signs of increased intracranial pressure, or seizures), an MRI of the brain and/or spine is warranted to exclude central nervous system (CNS) causes (like demyelinating disease or tumors). For example, fatigue coupled with neurologic changes could indicate multiple sclerosis (which is rare in children but possible in teenagers) or a tumor affecting the hypothalamus (leading to apathy).
CT scans: Generally less useful for fatigue unless investigating a specific area (e.g., chest CT for suspected lymphoma after abnormal X-ray or abdominal CT for mass).
In many cases of fatigue, initial imaging may be normal or unnecessary. The decision to perform imaging should be guided by clinical findings—for instance, don’t order a brain MRI for every tired child, but do so if focal neurologic signs or severe headaches are present. Similarly, avoid excessive radiation; utilize ultrasound or MRI when appropriate for joints and soft tissues.
When to Refer to Pediatric Rheumatology
Primary care providers frequently initiate workups, but knowing when to refer to a pediatric rheumatologist can significantly influence outcomes. An early referral is advisable if you suspect an underlying rheumatologic disease or if the initial evaluation presents concerning signs that require specialist management. Refer to pediatric rheumatology in the following scenarios:
Persistent Arthritis: Any child with objective joint swelling or stiffness lasting >6 weeks should be referred for evaluation of JIA. This includes:
Swollen joint(s) on exam that is not explained by trauma or infection.
Chronic limp or joint contracture develops over time.
Persistent back pain with stiffness, significantly if worse in the morning (suspicious for juvenile spondyloarthropathy).
Even without noticeable swelling, if a child has significant morning stiffness or activity limitation due to joint pain for weeks, refer for possible inflammatory arthritis.
Suspected Lupus or Multi-System Autoimmune Disease: Refer promptly if a child has multi-system involvement suggestive of SLE or related connective tissue disease. For example:
- Malar rash or another lupus-specific rash that is not transient.
- Positive ANA plus clinical signs (arthritis, proteinuria, oral ulcers, cytopenias, serositis, neurologic symptoms). Note: Do not refer solely to a positive ANA without clinical correlation – instead, evaluate for signs first. However, a comprehensive rheumatologic evaluation is required if ANA is accompanied by any other lupus features.
- Unexplained nephritis (proteinuria, hematuria) or other organ inflammation (e.g., pericarditis) in a child presenting with fatigue could indicate lupus or vasculitis.
- Prolonged fever with rash and arthritis (systemic JIA, lupus, or autoinflammatory) – if infection and malignancy are ruled out, refer to rheum.
Dermatomyositis / Muscle Weakness: If you identify proximal muscle weakness not due to an evident neurologic disorder, significantly if skin changes such as Gottron papules or heliotrope rash are present, urgent referral to rheumatology is indicated. Rheumatology can coordinate confirmation (e.g., MRI or biopsy) and initiate therapy for JDM. Even if the rash is absent but there’s unexplained high CK and weakness, rheumatology can help differentiate inflammatory myositis from other myopathies. Generally, any child with confirmed elevated muscle enzymes and weakness should see a rheumatologist or neurologist; rheumatology is the appropriate choice call if rash or other autoimmune features are present.
Vasculitis or Other Rare Rheumatic Disease: Refer if you suspect vasculitis (e.g., characteristics of Takayasu: limb blood pressure discrepancy, absent pulse, or systemic vasculitic rash with fever).
Recurrent fevers with inflammation: If a child has periodic fever episodes with systemic symptoms (and workups have excluded infection), refer for periodic fever syndromes or systemic JIA evaluation. Pediatric rheumatology can perform specialized testing and begin empiric treatments (like IL-1 blockers for suspected autoinflammatory syndromes).
Complex or Uncertain Cases: If, despite your initial workup, the cause of the child’s fatigue and weakness remains unclear, but you have some suspicion of an inflammatory or autoimmune process (for instance, perhaps only a high ESR and vague pains), a rheumatology consult can be very helpful in sorting it out. Rheumatologists are skilled in evaluating atypical presentations of rheumatic diseases and can also help rule out those disorders so you can pursue other options for causes.
Before initiating specific treatments: If you strongly suspect a rheumatologic condition requiring immunosuppressive therapy (such as high-dose steroids, methotrexate, or biologics), involve rheumatology immediately. For example, suppose you suspect juvenile dermatomyositis (JDM) and observe a high creatine kinase (CK). In that case, you might initiate steroids empirically, but it is ideal to consult with rheumatology and arrange for a prompt referral (often, these patients are seen emergently).
If you feel out of depth: Pediatric rheumatologists are skilled at guiding evaluations. If fatigue or malaise significantly impacts a patient’s quality of life and no underlying cause is identified, a rheumatologist may help confirm the presence of subtle rheumatic diseases or recognize a condition like fibromyalgia that can be treated with their expert input.
When referring, provide the consultant with your findings: growth charts, a summary of key history, exam signs (such as rash descriptions and which joints are swollen), and lab results completed so far (including CBC, ESR, etc.). This helps them assess the urgency. For example, suspected lupus with renal issues is urgent (they may want to see the patient within days), whereas mild chronic fatigue with a positive ANA but no other findings might be routine. If a patient is acutely very ill (e.g., high fever, possible macrophage activation syndrome, or rapidly progressive weakness), coordinate an urgent or inpatient referral – many pediatric rheumatologists will accept a direct call from the pediatrician in such scenarios.
Do not hesitate to refer if the criteria are met; early specialist involvement for diseases such as JIA, lupus, or JDM enhances outcomes by preventing organ damage and growth complications. Conversely, if you are pretty sure that the fatigue is due to a non-rheumatic cause (e.g., depression or lack of sleep), address those issues first and consider rheumatology referral only if symptoms do not improve or if new findings arise.
Conclusion
Evaluating children’s weaknesses, fatigue, and malaise requires a broad differential and methodical approach. Begin with common causes (anemia, thyroid disease, sleep issues) but maintain a high degree of suspicion for severe conditions. Pediatric rheumatologic diseases—though less common—are significant causes of chronic fatigue and weakness that often present with subtle early signs. By gathering key historical details (including psychosocial factors), performing a focused physical examination (looking for rashes, joint findings, and muscle strength), and ordering first-line investigations, a general pediatrician can identify most red flags that indicate a rheumatologic or other organic illness. Early referral to pediatric rheumatology is necessary when clinical criteria suggest an inflammatory cause requiring specialized care. In children without red flags and a normal initial workup, a prudent period of observation with supportive care is reasonable, along with follow-up to ensure improvement or detect any emerging signs.
Above all, maintain a holistic perspective: the cause of pediatric fatigue is often multifactorial. It may involve a combination of a mild medical issue (e.g., low iron) and lifestyle factors. Address each contributing factor—correct deficiencies, treat inflammation and optimize sleep and mental health. By doing so, you will help restore the child’s energy and functionality. If an actual pediatric rheumatologic condition is present, recognizing it early and collaborating with a specialist will place the child on the best path for management, improving their long-term outcome and quality of life.
Essential Academic Papers:
General Approach to Pediatric Fatigue
De Nardi L, Lanzetta MA, Ghirigato E, Barbi E, Gortani G. Approach to the child with fatigue: A focus for the general pediatrician. Front Pediatr. 2022; 10:1044170. DOI: 10.3389/fped.2022.1044170
Findlay SM. The tired teen: A review of the assessment and management of the adolescent with sleepiness and fatigue. Paediatr Child Health. 2008; 13(1):37–42. DOI: 10.1093/pch/13.1.37
Non-Rheumatologic Causes of Pediatric Fatigue
Brigden A, Loades ME, Abbott A, Bond-Kendall J, Crawley E. Practical management of chronic fatigue syndrome or myalgic encephalomyelitis in childhood. Arch Dis Child. 2017; 102(10):981–986. DOI: 10.1136/archdischild-2016-310622
Katz BZ, Shiraishi Y, Mears CJ, Binns HJ, Taylor R. Chronic fatigue syndrome after infectious mononucleosis in adolescents. Pediatrics. 2009; 124(1):189–193. DOI: 10.1542/peds.2008-1879
Loades ME, Read R, Smith L, Higson-Sweeney NT, Laffan A, et al. How common are depression and anxiety in adolescents with chronic fatigue syndrome (CFS) and how should we screen for these co-morbidities? A clinical cohort study. Eur Child Adolesc Psychiatry. 2021; 30(11):1733–1743. DOI: 10.1007/s00787-020-01646-w
van de Vijver E, van Gils A, Beckers L, van Driessche Y, Moes N, van Rheenen PF. Fatigue in children and adolescents with inflammatory bowel disease. World J Gastroenterol. 2019; 25(5):632–643. DOI: 10.3748/wjg.v25.i5.632
Carroll S, Chalder T, Hemingway C, Heyman I, Moss-Morris R. Understanding fatigue in paediatric multiple sclerosis: a systematic review of clinical and psychosocial factors. Dev Med Child Neurol. 2016; 58(3):229–239. DOI: 10.1111/dmcn.12964
Nacul LC, Kingdon CC, Bowman EW, et al. Myalgic encephalomyelitis/chronic fatigue syndrome diagnosis and management in young people: a primer. Front Pediatr. 2017; 5:121. DOI: 10.3389/fped.2017.00121
Rheumatologic Causes of Pediatric Fatigue
Avar-Aydın PÖ, Brunner HI. Revisiting childhood-onset systemic lupus erythematosus. Turk Arch Pediatr. 2024; 59(4):336–344. DOI: 10.5152/TurkArchPediatr.2024.24097
Armbrust W, Lelieveld OHTM, Tuinstra J, Wulffraat NM, Bos GJF, et al. Fatigue in patients with juvenile idiopathic arthritis: relationship to perceived health, physical health, self-efficacy, and participation. Pediatr Rheumatol. 2016; 14:65. DOI: 10.1186/s12969-016-0125-1
Kobayashi I. Advances in juvenile dermatomyositis: pathophysiology, diagnosis, treatment and interstitial lung diseases – a narrative review. Children (Basel). 2024; 11(9):1046. DOI: 10.3390/children11091046
Ozen S, Sag E. Childhood vasculitis. Rheumatology (Oxford). 2020; 59(Suppl 3):iii95–iii100. DOI: 10.1093/rheumatology/kez599
Kant-Smits K, van Brussel M, Nijhof SL, van der Net J. Reducing fatigue in pediatric rheumatic conditions: a systematic review. Pediatr Rheumatol. 2021; 19:111. DOI: 10.1186/s12969-021-00580-8
Cross-Cutting Overviews and Comparative Studies
Crichton A, Knight S, Oakley E, Babl FE, Anderson V. Fatigue in child chronic health conditions: a systematic review of assessment instruments. Pediatrics. 2015; 135(4):e1015–e1031. DOI: 10.1542/peds.2014-2440
Sharpe M, Wilks D. Fatigue. BMJ. 2002; 325(7362):480–483. DOI: 10.1136/bmj.325.7362.480